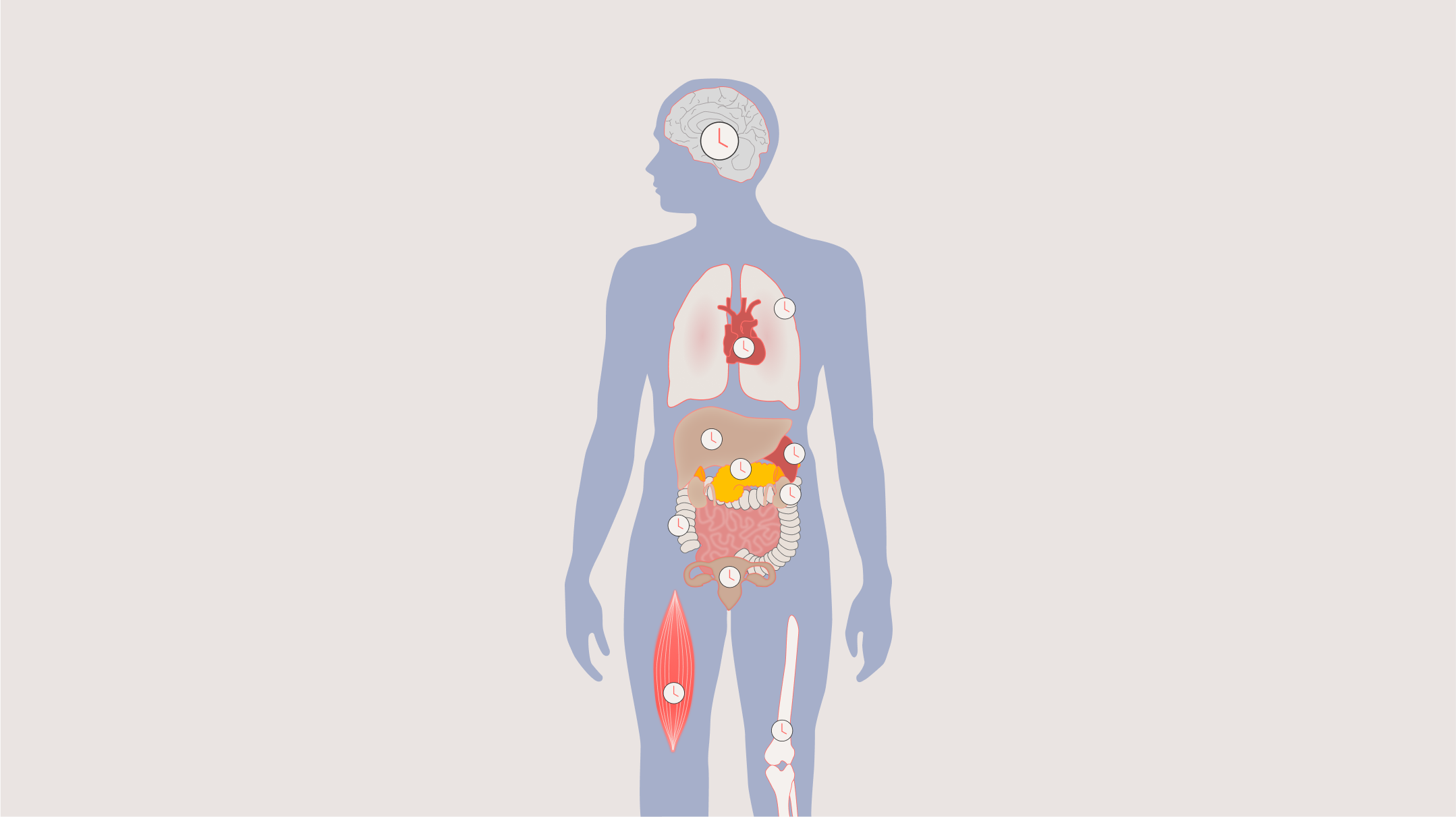
Why medication timing matters
Modern medicine is exacting about what you take and how much. But it pays almost no attention to when you take it — and a growing body of evidence suggests that timing may be one of the most overlooked variables in treatment effectiveness.
The reason is circadian biology. Nearly every organ in your body operates on a roughly 24-hour cycle, governed by molecular clocks that regulate everything from hormone secretion and immune activity to how your liver metabolizes drugs. These rhythms determine when a drug’s target is most active, when your body can best absorb and process a compound, and when healthy cells are most or least vulnerable to toxic side effects.
That means the same pill, taken at 8 a.m. versus 8 p.m., may work very differently — not because the drug has changed, but because you have.
What the research shows
A landmark review published in Science in 2019 analyzed 106 clinical trials across 50 years and found that in 75% of cases, treatment efficacy or toxicity varied depending on dosing time. The conditions affected include some of medicine’s most common and costly: hypertension, cancer, asthma, and arthritis.
For drugs with shorter half-lives — those that are absorbed and cleared relatively quickly — the effect was even more pronounced. Among drugs with half-lives under 15 hours, 85% showed dosing-time dependence. The authors noted that this insight alone could determine whether a drug receives FDA approval.
Yet despite these findings, only four of the 50 most commonly prescribed drugs in the United States carry an FDA-approved recommendation for when they should be taken. The World Health Organization’s Model List of Essential Medicines makes no mention of dosing time at all.
Why short-acting drugs are more time-sensitive
The logic is straightforward. A drug that remains active in your body for 24 hours or more will be present regardless of when you take it. But a drug that peaks and clears within a few hours creates a narrow window — and whether that window aligns with the optimal circadian phase of its target can make or break its effectiveness.
This explains some seemingly contradictory results in the research literature. Simvastatin, a short-acting cholesterol drug with a half-life of about three hours, consistently works better when taken in the evening — because the enzyme it inhibits peaks at night. But atorvastatin, a longer-acting statin with a half-life of 25 hours, shows no meaningful morning-versus-evening difference. The drug is always present, so timing matters less.
The same pattern holds across drug classes. Short-acting blood pressure medications, for example, tend to be more effective when taken at bedtime — and better at restoring the natural overnight dip in blood pressure that is protective against cardiovascular events. Longer-acting formulations often mask these circadian effects entirely.
Vaccines work better at certain times too
The immune system is one of the most strongly circadian systems in the body. Immune cells are primed for rapid response during waking hours and shift to surveillance and information-processing mode during sleep. This has practical consequences for vaccination.
Research has shown that the time a vaccine is administered can meaningfully influence the strength of the immune response. A study examining the BCG vaccine found that participants vaccinated in the morning (8–9 a.m.) mounted a significantly stronger immune response — with higher levels of key cytokines — than those vaccinated in the late morning or evening, and that this advantage persisted for at least 12 weeks.
Similar findings have been reported for influenza vaccines, where morning vaccination has been associated with higher antibody titers compared to afternoon vaccination. Given the scale of global vaccination programs, even modest improvements in immune response from time-of-day scheduling could have an outsized public health impact.
The missing variable: your internal clock
Most of the research to date has tested treatments at fixed clock times — 8 a.m. versus 8 p.m., for example. This approach has been valuable, but it has a fundamental limitation: it assumes all patients are on the same internal schedule.
They are not. Studies have shown that the timing of dim light melatonin onset (DLMO) — a reliable marker of an individual’s circadian phase — varies by five to six hours even under controlled laboratory conditions. In real-world populations, the range is even wider: up to nine hours in university students and twelve hours in shift workers.
This means that a drug prescribed for “8 a.m.” may reach two patients at very different points in their circadian cycle. One may be receiving it near the peak of its efficacy window. The other may be missing that window entirely — and neither patient nor physician would know the difference.
What this means for the future
Circadian medicine takes the concept of timed dosing a step further. Rather than prescribing treatments based on clock time, the goal is to align them with each individual’s internal circadian phase — the point in their personal biological cycle when a drug, vaccine, or therapy would be most effective or least toxic.
For existing medications, circadian-informed dosing could improve outcomes without changing the drug itself. For drugs in clinical development, incorporating timing data could reduce toxicity-related trial dropouts, sharpen results, and improve approval odds. And for patients, it could mean fewer side effects and better results — simply by shifting when a treatment is delivered.
The science of drug timing is no longer theoretical. It is supported by decades of clinical data and increasingly understood at the molecular level. The question is no longer whether timing matters — it is how quickly medicine will begin to act on it.
References
- Ruben et al. (2019) — Dosing time matters. Science.
- Cederroth et al. (2019) — Medicine in the fourth dimension. Cell Metabolism.
- De Bree et al. (2020) — Non-specific effects of vaccines: current evidence and potential implications. Journal of Clinical Investigation.
- Van Diemen et al. (2020) — Chronotherapy of conventional low-dose aspirin in healthy volunteers. Platelets.
- Sletten et al. (2015) — Inter-individual differences in neurobehavioural impairment following sleep restriction are associated with circadian rhythm phase. PLoS One.
- Phillips et al. (2017) — Irregular sleep/wake patterns are associated with poorer academic performance and delayed circadian and sleep/wake timing. Scientific Reports.
- Dumont et al. (2001) — Profile of 24-h light exposure and circadian phase of melatonin secretion in night workers. Journal of Biological Rhythms.